
 Tami Neumann
Tami Neumann
Tami is passionate about creating an informed and connected community. Curating conferences and creating dynamic educational content that provide the community a welcoming place to learn and grow is important to Tami, she feels this is paramount to creating a culture shift in the aging space. As a Certified Dementia Practitioner, Tami has spent over 20 years in the Aging Industry. In her free-time you will find her advocating for people with Type 1 Diabetes and developing her skills in improv.  Catherine Braxton
Catherine Braxton
Catherine is passionate about providing education in a format that is engaging, fun and digs deep. Her educational background in psychology lays the foundation for each module that is crafted in such a way that will immerse you fully in its content. In 2015, she began offering workshops and seminars through Prairie State College. Catherine has spent the past 20 years in the aging industry managing memory care units, providing activities as a case manager. Tami and Cathy came to a BrightStar Care event to share some tips on using improv techniques to better communicate with Dementia Care Patients. Here's are the tips: 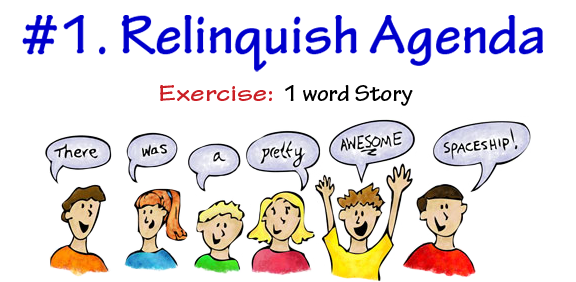 When doing this exercise, it is important that each person only state 1 word each until the next round. Now try and make a story!
When doing this exercise, it is important that each person only state 1 word each until the next round. Now try and make a story! When Tami and Cathy asked each volunteer how they felt their responses were:
-I felt put on the spot
- it was very challenging
- It was hard to think ahead
- You have to think fast on your feet
It is IMPORTANT to remember that as a CAREGIVER you need to Relinquish your Agenda! Your need to be right doesn’t create a connection and when trying to communicate with Dementia patients...you need a connection. Let’s pretend your friend comes to you and just wants to vent...you’re already thinking of advice or ways to help her...but what if she JUST wants you to listen.Cathy calls this “Hold the Bucket” = just listen
So remember: let go of your need to be right, get rid of your agenda and just LISTEN.

Partner: can be care partner, spouse, patient etc...
The goal is to make your partner look good by NOT putting them in shame, giving them any heavy lifting, or making negative judgments. So what does that mean?
Let’s take a look at THANK YOU VS. I’M SORRY
Thank you = positive I’m sorry = heavy lifting

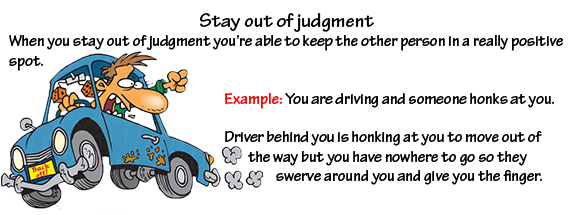 Your initial reaction is to get upset and you think “wow, what a jerk” Now, you don’t know why that driver was in such a hurry or why they seemed upset but what if they just received a call that their mom is in hospice and doesn’t have much time left to live. They are obviously going to try to get there as fast as they can. Instead of making a negative judgment try to make a positive one. It’ll make YOU feel better by not assuming the negative. The stories we make up are wrong anyway so why not make them positive. Make people you don’t know look good too. When you judge it’s usually for the negative.
Your initial reaction is to get upset and you think “wow, what a jerk” Now, you don’t know why that driver was in such a hurry or why they seemed upset but what if they just received a call that their mom is in hospice and doesn’t have much time left to live. They are obviously going to try to get there as fast as they can. Instead of making a negative judgment try to make a positive one. It’ll make YOU feel better by not assuming the negative. The stories we make up are wrong anyway so why not make them positive. Make people you don’t know look good too. When you judge it’s usually for the negative. Strive to be positive!

What are “The Gifts?”
When working with a person with Dementia, you should be consistently looking for the gifts they’re giving you to be able to communicate with them in a positive way.“I want to go home” is a common statement that you’ll hear from someone who has Dementia.
 The gift in that sentence is Home.
The gift in that sentence is Home. Reality Orientation
You may know it’s 2016 but Mrs. Smith may think it’s 1920 and often times caregivers try to pull the patient into THEIR reality. Home is something we shy away from because we don’t know how to answer that. We know it is not their home, we know they are in a negative space, that they don’t feel warm, comfortable, embraced…but all of those emotions can be related to home.Think of what brings you comfort.
People with dementia have memories of home... enter into their reality and ask them about their home. Look for the noun within the sentence, their emotion and their body language. Use these clues to discover the gift they are giving you and give THEM comfort.
Yes = Be in Agreement! And = Add something to it!
Improv is built on this rule.
Exercise: Ask questions and try to respond with a YES/ AND.
“I hear your mother is the bearded lady at the circus.”
- Yes and she likes to sing too.
That was a pretty straightforward way to answer with YES/AND.“Did you steal my corn?”
- No but I cut it up and left it in the microwave.
Even though the response starts with a “no” this is still a YES/AND because the answer is still in agreement.“I don’t want to shower, it’s winter in there, I don’t want to shower.”
-Why don’t we turn the water on and make sure it’s warm so you don’t feel cold.
Clue: Winter = it’s cold
"Did you see the little boy? I think he’s going to get hurt.”
-I don’t see him, but let’s go try to find him.
“It’s time for me to go because I have to pick up the children.”
-Isn’t it so exciting that we get to pick up our kids from school, how old are they?
And with that you can start a conversation… You can also YES/AND with touch. If you see someone acting anxious or fidgeting with their hands you could hold their hand and place your other hand over theirs. This is how you could physically YES/AND someone. YES/AND when walking: If someone is pacing frantically, match their pace and try to slow down…they will mirror you and slow down as well. Don’t get caught up in the concept of saying yes. There is no right or wrong YES/AND response:“Do you see the monkeys in the backyard?”
-I don’t but how many are there?
Maybe the monkeys the person is seeing are shadows and you could possibly close the blinds...sometimes we see things that aren’t there. Start a conversation about monkeys and create some peak moments for success with your Dementia patient.“Have you seen my mother? I have to go find her.”
- When was the last time you saw her? What does your mother look like?
It’s safe to assume that the patient’s mother is no longer alive…the response is in agreement because it is acknowledging that the patient wants to see their mother. Create a response that will provide comfort to the person with Dementia.
